More than 140,000 Americans die from COPD each year – here’s why survival depends on more than avoid
Research shows that social isolation plays a major role in quality of life and risk of death in people with COPD.

Chronic obstructive pulmonary disease, or COPD, caused 141,733 deaths in the United States in 2023 – the latest data that has been reported. That number reflects not just the effects of smoking, but a broader set of medical and social factors that shape who survives.
As of early 2026, COPD remains the fifth-leading cause of death nationwide and carries a substantial economic burden, with annual medical costs estimated at US$24 billion among adults ages 45 and older. COPD is a progressive condition that limits airflow, making it increasingly difficult to breathe and carry out everyday activities.
Nearly 16 million U.S. adults live with COPD, and many more remain undiagnosed.
COPD also encompasses chronic bronchitis, which inflames the airways, and emphysema, a condition that damages the air sacs in the lungs. Both conditions limit the flow of air in and out of the lungs.
I am a physician and doctoral researcher in public health who studies chronic disease outcomes using nationally representative U.S. data. In my research examining long-term mortality among adults living with COPD, one pattern stands out clearly: My colleagues and I found that both current and former smokers had a higher risk of death compared with those who never smoked, highlighting that smoking increases mortality risk – but it does not act alone.
How smoking and COPD are intertwined
Smoking has been recognized for over five decades as the primary cause of COPD. It is a major factor in how the disease develops and progresses, although other factors such as secondhand smoke, air pollution and occupational exposures also play a role. Even after accounting for age and other health conditions, people with COPD who have smoked face a higher risk of death than those who have never smoked.
Quitting smoking, while essential, does not fully erase the damage caused by smoking. This is because long-term exposure to tobacco smoke leads to persistent inflammation and structural damage in the lungs, changes that are not fully reversible. They continue to affect airflow and respiratory function even after a person stops smoking, although quitting significantly slows further decline.
COPD is a long-term condition that continues to affect the lungs and the pulmonary blood vessels over time, contributing to both breathing problems and other chronic conditions.
In some cases, higher risks among former smokers with COPD may reflect the lasting effects of smoking or underlying illness that led them to quit.
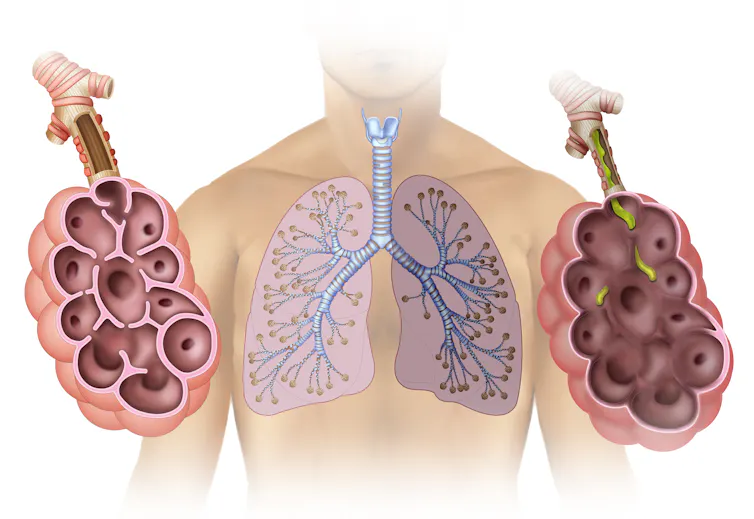
COPD affects more than the lungs
COPD is often described as a lung disease, but its effects extend far beyond breathing.
People living with COPD also face a higher risk of other health problems, including lung infections such as flu or pneumonia, lung cancer, heart disease, weak muscles and depression or anxiety, all of which can increase the risk of death.
One of the most noticeable ways COPD affects daily life is through persistent breathlessness, which can make even simple tasks such as walking, cooking or getting dressed more difficult. As activity declines, overall health can worsen, creating a cycle that is hard to break.
COPD is also frequently diagnosed late and progresses gradually, limiting opportunities for early treatment.
Social connections can shape survival
A growing body of research shows that social factors play a meaningful role in health outcomes with chronic diseases including COPD. Social isolation has been linked to a higher risk of premature death, with effects comparable to well-known risk factors such as smoking and obesity. This is a major problem because nearly 1 in 6 adults with COPD experience social isolation, and 1 in 5 experience loneliness.
Among people living with COPD who were single or never married, the increase in overall risk of death associated with smoking was substantially higher. In this socially isolated group, current smokers faced roughly a 50% higher risk of death and former smokers faced nearly four times the risk compared with those who never smoked, highlighting how social context can shape survival rates.
Other research has similarly found that social isolation is associated with a higher risk of death among people with COPD, reinforcing the importance of social support. Managing a demanding chronic illness alone can be difficult; without support to monitor symptoms or assist with care, the burden of disease may be grave.
One reason is that social connections influence how people manage chronic illnesses. People who are socially isolated are more likely to engage in unhealthy behaviors such as smoking, poor diet and physical inactivity, and may be less likely to follow treatment plans.
Support from family members, caregivers or community networks can improve peoples’ likelihood of following treatments, reduce their stress and make it easier to quit smoking. For people living with COPD, a condition that requires daily management, these differences can significantly affect their quality of life and how long they live.
What can help reduce COPD deaths?
Reducing deaths from COPD begins with prevention and early intervention. Avoiding or quitting smoking remains the most effective way to lower risk. Reducing exposure to tobacco smoke, air pollution and occupational hazards such as dust from mining and chemical fumes can also help prevent long-term lung damage.
For people already living with COPD, consistent access to care can improve outcomes. Treatments such as inhalers that help open the airways, pulmonary rehabilitation and oxygen therapy, along with vaccinations against respiratory infections, can help manage symptoms and reduce complications.
Improving survival in COPD depends on more than treatment alone – it also requires addressing social factors such as isolation, access to support and living conditions.
One practical step is making screening for social isolation part of routine care.
Olamide Asifat does not work for, consult, own shares in or receive funding from any company or organization that would benefit from this article, and has disclosed no relevant affiliations beyond their academic appointment.
Read These Next
Today’s bans on DIY repairs of everything from cell phones to tractors grew out of Hollywood’s fear
Efforts to use technology to police copyright evolved into companies using copyright law to lock people…
Why Corpus Christi faces a looming water shortage, and what might help
Years of industrial expansion have boosted water demand, with no new sources coming online since 2016.…
America’s nonprofit sector is pushing back against an ‘authoritarian playbook’
The Trump administration has made many threats against nonprofits whose missions it disagrees with.





